Scientists modify antibiotic to create new super-strength drug to fight deadly superbugs
Vancomycin is known as an 'antibiotic of last resort' due to its power to treat serious infections when other drugs have failed
Scientists have boosted the strength of a key antibiotic used to fight superbugs – an advance they hope will help combat the threat of MRSA and other antibiotic-resistant infections.
The drug vancomycin is known as an “antibiotic of last resort” due to its power to treat serious infections when other drugs have failed.
Researchers have now re-engineered the medicine to work in three separate ways on bacteria, making it much harder for bugs to develop resistance to it.
A study carried out at The Scripps Research Institute (TSRI) in California suggests the new version of vancomycin is a thousand times stronger than the old drug, although it has not yet been tested in animals or humans.
Scientists are racing to develop a new generation of medicine capable of defeating even the most resistant superbugs, which represent an “increasingly serious threat to global public health,” according to the World Health Organisation.
Antimicrobial resistance is caused when bacteria, viruses, fungi and parasites change through continued exposure to drugs, which then become ineffective against them.
Over time, excessive use of antibiotics could lead to minor infections causing serious health complications, making surgery and treatment for diseases such as cancer much riskier.
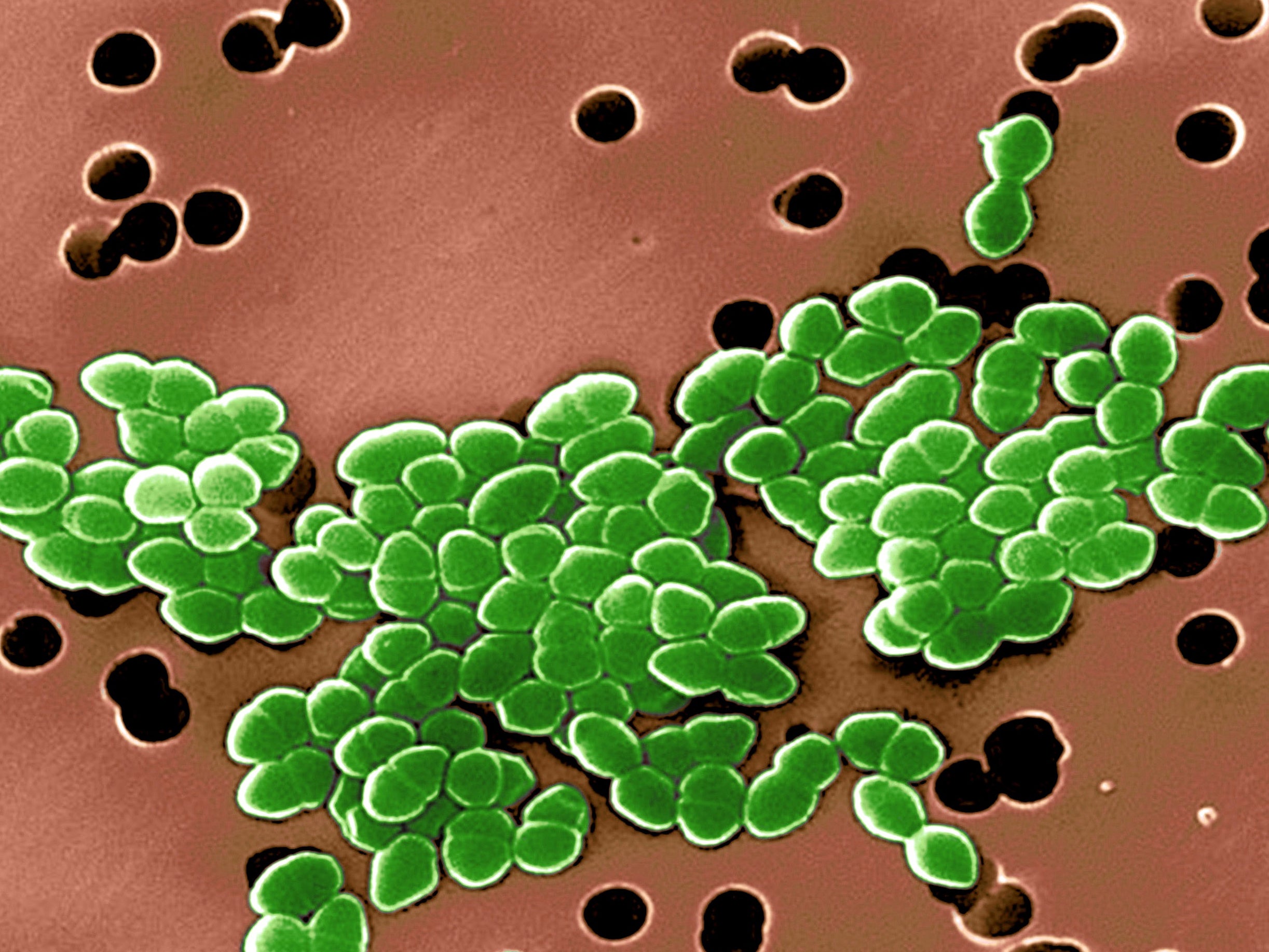
Vancomycin has been prescribed by doctors for 60 years, but bacteria are only now becoming resistant to it.
The length of time it has taken for resistance to develop suggests bugs have had a hard time overcoming the way the original drug worked – by disrupting how bacteria form cell walls – the researchers said.
Previous studies by the team showed it was possible to add two modifications to vancomycin, a drug they labelled “magical” because of its strength against infection, to make it even more potent and reduce the amount of the medicine needed to have the same effect.
The new study, published in the journal Proceedings of the National Academy of Sciences (PNAS), reveals another modification which interferes with bacteria cell walls in a different way.
Combined with the previous alterations, the latest modification gives vancomycin a 1,000-fold increase in activity, so doctors could use less of the antibiotic to fight infection, the researchers said.
It was tested on Enterococci bacteria and killed both vancomycin-resistant Enterococci - considered by the WHO to be one of the drug-resistant bacteria that pose the greatest threat to human health - and the original forms of Enterococci.
The research was led by Dale Boger, co-chair of TSRI's Department of Chemistry, who said the discovery made the new version of vancomycin the first antibiotic to have three independent “mechanisms of action” to kill bacteria.
“This increases the durability of this antibiotic,” he said. “Organisms just can't simultaneously work to find a way around three independent mechanisms of action. Even if they found a solution to one of those, the organisms would still be killed by the other two.”
England’s chief medical officer Dame Sally Davies has warned that 50,000 people die each year in Europe and the US from infections that have developed resistance against antibiotics.
“It is clear that we might not ever see global warming, the apocalyptic scenario is that when I need a new hip in 20 years I'll die from a routine infection because we've run out of antibiotics,” she told MPs.
Additional reporting from Press Association
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
Comments
Bookmark popover
Removed from bookmarks