NHS England launches trial of 'game-changing' HIV treatment after court ruling
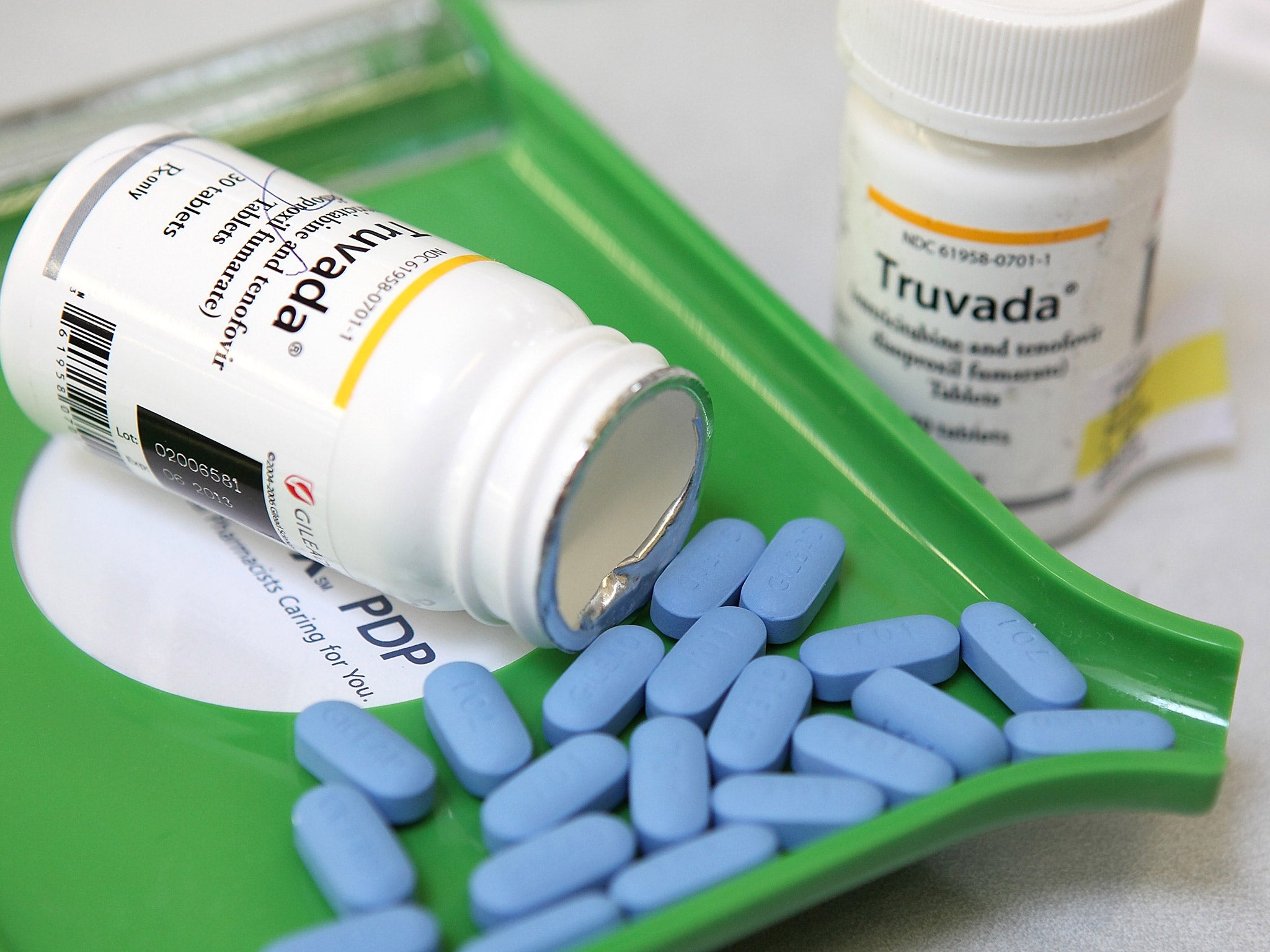
The treatment, known as PrEP, has been shown to reduce the risk of infection in people who are at high risk by more than 90 per cent
Your support helps us to tell the story
From reproductive rights to climate change to Big Tech, The Independent is on the ground when the story is developing. Whether it's investigating the financials of Elon Musk's pro-Trump PAC or producing our latest documentary, 'The A Word', which shines a light on the American women fighting for reproductive rights, we know how important it is to parse out the facts from the messaging.
At such a critical moment in US history, we need reporters on the ground. Your donation allows us to keep sending journalists to speak to both sides of the story.
The Independent is trusted by Americans across the entire political spectrum. And unlike many other quality news outlets, we choose not to lock Americans out of our reporting and analysis with paywalls. We believe quality journalism should be available to everyone, paid for by those who can afford it.
Your support makes all the difference.NHS England is launching a trial of the controversial HIV treatment PrEP after losing a Court of Appeal battle over who should fund it.
The drug, described as a “game changer” in the fight against HIV and Aids, has been shown to reduce the risk of infection in people who are at high risk by more than 90 per cent.
Last month, the Court of Appeal upheld a High Court ruling which said NHS England did have the power to fund the drug despite its pleas that the responsibility lie with local authorities.
Now, the organisation has announced it will fund “a large scale clinical trial in the early financial year 2017/18” for the drug, which has the brand name Truvada.
NHS England said that although the evidence around the clinical effectiveness of PrEP “is strong”, Public Health England (PHE) has highlighted potential issues with its rollout that need answering.
“These questions will be answered by the clinical trial, paving the way for full rollout”, NHS England said.
At least 10,000 people will be enrolled on the trial over the next three years, with NHS England footing the trial bill of up to £10m over three years. No decision has been made on how a more comprehensive future programme would be funded.
Dr Jonathan Fielden, deputy national medical director at NHS England, said the new trial had “in part, been made possible by the willingness of many pharmaceutical and device companies to come forward with lower and more responsible prices. Continuing this constructive joint working will enable us to fund more new drugs and treatments in the future”.
NHS England has also agreed to fund 10 new specialised treatments. But it said three treatments will not be funded due to poor cost-benefit. This includes second stem cell transplants for patients whose disease has got worse.
Professor Kevin Fenton, director of health and wellbeing at PHE, said: “Currently 13,500 people are living in the UK with undiagnosed HIV and we are still seeing around 5,000 new infections each year.
“Given we are in the fourth decade of this epidemic there are too many new infections occurring, and we need to use all tools available to save lives and money.
“We're delighted to be working in partnership with NHS England on this major new addition to the national HIV prevention programme. This comes after much planning and preparation to ensure we can successfully coordinate this extremely important and large scale clinical trial.”
Izzi Seccombe, from the Local Government Association, said: “We are pleased that NHS England has acted quickly and chosen to fund the commissioning of this trial and rollout of PrEP. We now want to stand united with the NHS to defeat the spread of HIV.
“PrEP is a ground-breaking method of treatment that has the potential to save lives and councils want to work with the NHS to help roll out the trial.”
Ian Green, chief executive of the Terrence Higgins Trust, said: “With 17 new HIV diagnoses made every day, we need to be bold and ambitious in our approach to HIV prevention - and this must include access to PrEP for all who need it.
“We welcome the fact that PrEP will be made available to 10,000 people who are at risk over three years. Preventing the spread of HIV is good news for everyone. Not only will this make a life-changing difference to each of these individuals by protecting them from an incurable and highly stigmatised condition, but for every person who would have become HIV positive without PrEP, the NHS will save £360,000 in lifetime treatment costs.
“However there are many questions that need to be answered about the proposed trial. We need to know how it will work in practice and understand how those at risk, no matter where they live, will be able to access PrEP.
“This trial alone does not provide the long-term stability that is needed - NHS England must make a commitment now that when the trial ends they will fully fund PrEP for all those who are at risk.”
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies
0Comments